FieldStrength MRI magazine
User experiences - April 2017
AUH at the forefront of MRI guidance in adaptive cervical cancer radiotherapy
The advantages of 3D MRI-guided brachytherapy in cervical cancer treatment are simply too important to be ignored, according to Prof. Tanderup, Aarhus University Hospital, Denmark. Her institute is at the forefront of implementing the GEC ESTRO recommendations for MRI guided brachytherapy, which were initiated by pioneers from Vienna, Leuven and Paris. She is currently Chair of the GEC-ESTRO Gynecological working group that has a pivotal role for 3D MRI-guided brachytherapy in the treatment of locally advanced cervical cancer.
“We consider brachytherapy essential for obtaining disease control in cervical cancer”

Kari Tanderup, PhD
Professor at Aarhus University Hospital and visiting professor at Medical University of Vienna. She is currently chairing the GEC-ESTRO gynaecology working group, coordinator of the EMBRACE study, and was a co-author of the GEC-ESTRO recommendations III and IV for 3D image-based brachytherapy for cervical cancer.

Jacob Christian Lindegaard, MD, DMSc
Associate professor and consultant oncologist at Aarhus University Hospital. He is past-chair of the GEC ESTRO committee and coordinator of the EMBRACE study.

Erik Morre Pedersen, MD, DMSc, PhD
Associate professor and consultant radiologist at Aarhus University Hospital. He is leading radiologist for implementation of MRI for radiotherapy at AUH. He was a co-author of the GEC-ESTRO recommendations IV for 3D image-based brachytherapy for cervical cancer.
Brachytherapy is key to cervical cancer radiation treatment at AUH
The radiotherapy department at Aarhus University Hospital (AUH) houses a Philips Ingenia 1.5T MR-RT system that is dedicated for MRI simulation. In addition, access to another Ingenia 1.5T and an Ingenia 3.0T is secured for most of the brachytherapy procedures. MRI-guided pulsed dose rate (PDR) and high dose rate (HDR) brachytherapy have become routine procedures, with 1-4 patients per week receiving PDR brachytherapy for gynecological cancer or HDR brachytherapy for prostate cancer.
The advanced MRI-guided gynecological brachytherapy workflow at AUH is based on an extensive and long term collaboration in a multidisciplinary clinical and research team, which is supervised by radiation oncologist Jacob C. Lindegaard, radiologist Erik Morre Pedersen and medical physicist Kari Tanderup. The team has worked together on development of MRI-guided brachytherapy at AUH since 2004, and is currently involved in international recommendations, prospective clinical studies, functional imaging as well as teaching and workshops.
“We are convinced that brachytherapy is essential for obtaining disease control in cervical cancer,” says Kari Tanderup, PhD. “The combination of external beam radiation therapy (EBRT) and MR image-guided adaptive brachytherapy is our standard of care at AUH for the treatment of locally advanced cervical cancer.”
Clinical studies demonstrate survival benefit with brachytherapy
“By adding brachytherapy to the treatment of cervical cancer, much higher doses of radiation can be delivered to the tumor than by using EBRT alone.

Aarhus University Hospital, is a large teaching hospital with 1,150 beds and 10,200 employees. The oncology department offers specialized cancer therapy to more than 12,000 patients annually and a total of 53,000 radiotherapy treatments are performed on a yearly basis. The radiotherapy department includes 12 linear accelerators with on-board imaging, 3 brachytherapy afterloaders, as well as CT, MRI and PET/CT scanners dedicated to radiotherapy planning.
Two important papers from 2013 and 2014, based on North American databases of cervical cancer patients, have demonstrated that without brachytherapy boost, the overall survival is inferior by about 10%,” says Dr. Tanderup [1,2].
Han et al. compared brachytherapy plus EBRT with EBRT alone to treat cervical cancer for a group of 7359 patients. It was found that addition of brachytherapy to EBRT resulted in a greater than 10% increase in both 4-year cause-specific survival and overall survival [1].
As Dr. Tanderup says, “Looking at this evidence it seems unacceptable to not include brachytherapy in the treatment of locally advanced cervical cancer.”
“Moving to 3D MR-guidance can further improve local control”
MR imaging enhances the visualization of tumor response
Historically, brachytherapy dose was prescribed using 2D planning based on radiographs. A transition to 3D image-guided adaptive brachytherapy allows assessment of tumor regression during radiotherapy and conformation of the radiation dose to the residual tumor in an individualized, adaptive approach. “Using brachytherapy allows us to deliver a higher dose to a relatively small residual tumor. Many tumors show rapid regression, which means that huge changes take place during the first week of EBRT.
“Moving to 3D MRI-guidance in brachytherapy can further improve local control”, says Dr. Tanderup. “Understanding why MRI is important in adaptive brachytherapy, requires to first understand how definitive radiotherapy is administered in cervical cancer.
Treatment starts with EBRT. We are treating essentially three different targets. Both the target related to the primary tumor in the cervix and the prophylactic lymph node target are treated with 45-50 Gy. Then about half the patients have one or more pathologic lymph nodes that receive an EBRT boost dose of 55-60 Gy. We add brachytherapy to boost the residual target volume in the cervix, parametria and uterus [3].”
This is why we start brachytherapy either towards the end or even after EBRT, so after that major shrinkage.” “In order to identify the target and adapt the brachytherapy boost to the tumor response in an individual patient, we need an imaging modality that is able to visualize tumor regression. To achieve the best possible definition of the target volume, as well as organs at risk like the bladder and rectum, we need the excellent soft tissue contrast that we get with MRI.
The adaptive target concept is based on identification of three target volumes which are at different risk of recurrence. These target volumes are described in detail in the ICRU report 89 [4]:
1) residual gross tumor volume (GTVres), 2) high risk clinical target volume (CTVHR) including the GTVres, the cervix and residual parametrial infiltration and 3) intermediate risk CTV (CTVIR) which is related to the extension the initial GTV.
For example, around 70% of our patients have parametrial infiltration at diagnosis. When the tumor regresses, it leaves certain grey zones in the parametrium that cannot be discriminated by CT. We need MRI to see these grey zones as well as the GTVres ” says Dr. Tanderup. “The functional capabilities of MR, for instance DWI and DCE, may help further in visualizing the tumor and assessing response [5], but this is still under investigation.”
“Half the morbidity and 10% improvement in overall survival. It's a big difference!”
Image-guided brachytherapy for cervical cancer adds further 10% survival benefit
Dr. Tanderup has been deeply involved in the design and initiation of the EMBRACE studies together with Richard Pötter (PI of EMBRACE, Medical University of Vienna), Jacob Lindegaard (AUH) and Christian Kirisits (Medical University of Vienna). The EMBRACE studies have been designed to evaluate the clinical outcome of image guided brachytherapy in locally advanced cervical cancer [6].
“In parallel to the prospective, multi-center EMBRACE I study on MRI-guided therapy in cervical cancer, we also initiated a retrospective study called retroEMBRACE with 780 patients accrued or treated before the EMBRACE I study,” Dr. Tanderup explains.
“Recent results of the retroEMBRACE study report an additional 10% increase in overall survival compared to conventional brachytherapy [7]. That’s on top of the advantage of applying brachytherapy as such.
At the same time, mono-institutional series have demonstrated a major morbidity decrease to half of what it was with standard brachytherapy, says Dr. Tanderup [8-11].”
International consensus on 3D image guided brachytherapy
“These recommendations are now also embedded in the recently published ICRU report, which explains in detail how to define the target, how to report, and how to use clinical examination and 2D or 3D images for disease assessment and treatment planning,” says Dr. Tanderup. “With this international consensus, the approach is ready for international dissemination.” [4]
The pivotal role of MRI for the successful implementation of 3D image-based brachytherapy for cervical cancer has been underscored in the recommendations of the GEC-ESTRO Working Group, that Dr. Tanderup currently chairs [12-15].
MRI is important at all stages of cervical cancer radiotherapy
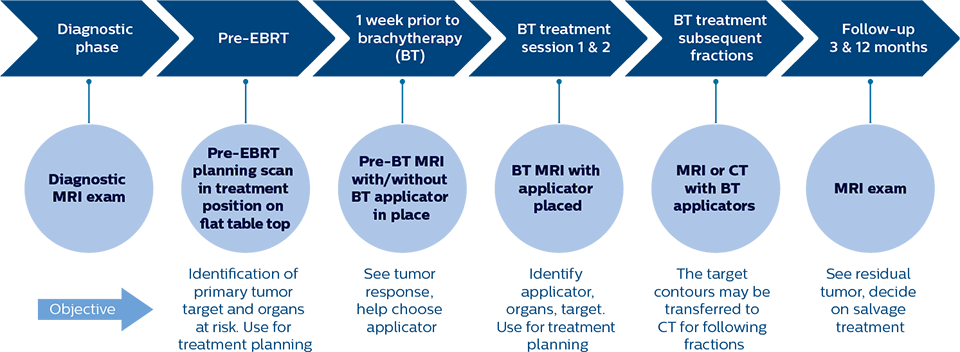
At AUH, MRI plays a role across the entire patient trajectory for cervical cancer radiation therapy patients. “Our workflow is closely based upon the GEC-ESTRO guidelines,” says Dr. Tanderup.
“In patients referred for cervical cancer treatment at our hospital, MRI has already been part of the diagnostic process. Before initiation of EBRT, PET-CT and MR treatment planning scans are acquired with the patient in treatment position on flat table top.
The images are fused and used for MRI-guided target definition of the primary tumor and for PET-guided definition of pathological lymph nodes.
Then we perform pre-brachytherapy MRI within one week before the first brachytherapy session. This MRI exam is done with a dummy applicator in place to establish the geometry we are going to see at brachytherapy. This MRI exam allows us to see how the tumor responded to EBRT and we also use it to decide which kind of applicator the patient needs. For instance, if we see a very advanced tumor with poor regression, we need a more advanced applicator which combines intracavitary and interstitial brachytherapy.”
At Aarhus, MRI plays a role across the entire patient trajectory for cervical cancer radiation therapy
“Brachytherapy dose calculation can be based directly on MRI without any problem”
Case study: MR-guided brachytherapy in patient with cervix cancer
Patient history
Stage IIB cervix cancer patient with a primary tumor with width of 6.0 cm and proximal/distal infiltration of left/right parametria at diagnosis. The patient had one PET-positive external iliac lymph node.
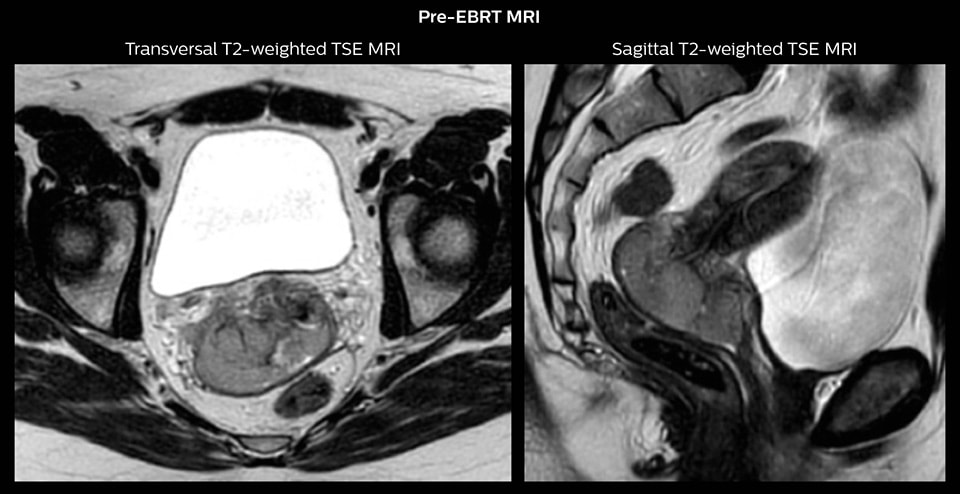
The patient was treated with external beam radiotherapy (EBRT) and concomitant chemotherapy. EBRT was delivered as IMRT with daily IGRT and a total dose of 45 Gy in 25 fractions to the pelvis and 55/25 fractions to the PET-positive lymph node. There was good tumor response during therapy and towards the end of EBRT the primary tumor had regressed to 3.8 cm width and proximal parametrial infiltration.
Brachytherapy
Two pulsed dose rate (PDR) brachytherapy fractions were delivered after end of EBRT in weeks 6 and 7.
One week prior to the first brachytherapy fraction, pre-planning was performed. Pre-planning involved insertion of intracavitary tandem-ring applicator and MR imaging with applicator in place.
An MRI-based pre-plan was carried out to determine the number, position and length of needles to be implanted through the ring applicator. Brachytherapy was delivered with the tandem ring applicator combined with 6 interstitial plastic needles.
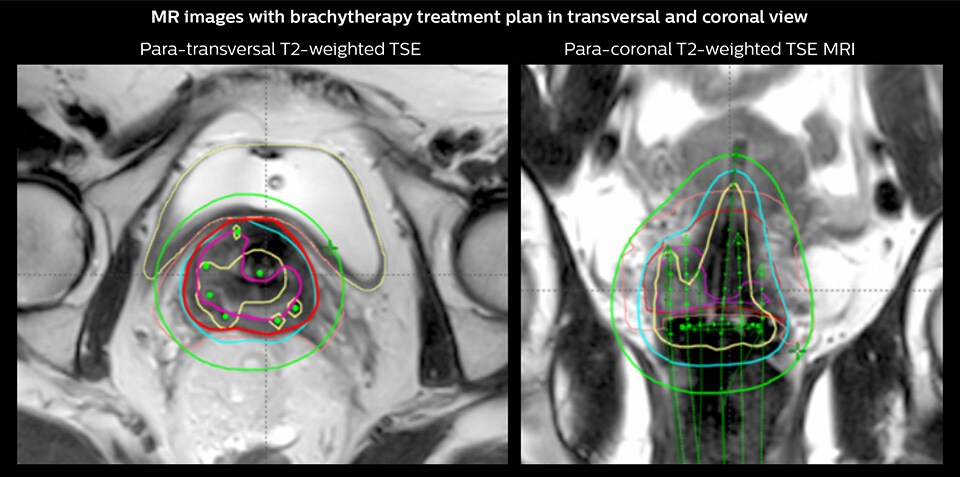
Red CTVHR; Pink residual GTV; Yellow 200% isodose; Cyan 85 Gy EQD2 isodose; Green 60 Gy EQD2 isodose; Green applicators, needles
Brachytherapy dose calculation based on MRI
“On the treatment day we insert the brachytherapy applicator, which has channels that go into the uterus and in the upper vagina just below the cervix. We may have additional needles targeting the parametrial infiltration. At Aarhus we use an MR-compatible applicator based on a tandem-ring system with a cap with holes for guidance of interstitial plastic needles. We also use individualized 3D-printed applicators when needed. With the applicator in place we then perform another MRI exam. These images are used to help us identify the applicator, the organs and the target. And we use them to do the treatment planning,” says Dr. Tanderup.
“Both target and organ delineation as well as dose calculations can be based directly on the MR images. With external beam radiation therapy, dose calculations are based on x-ray attenuation derived from CT. However, brachytherapy dose calculation is performed in a simpler way and can be based directly on MRI without any problem.”
“Everything takes place according to a dense schedule in one day: applicator implantation, MR imaging, treatment planning, and initiation of delivery. The patient stays overnight with the applicator in place as we deliver PDR brachytherapy over 20 hours. The applicator is then taken out and the second fraction is delivered the following week.”
“Brachytherapy does not depend on the patient position in the same way as EBRT since the irradiator is inside the patient. Therefore, we can image our patients on the diagnostic couch top. For MRI-guided HDR prostate brachytherapy we use the FlexTrak patient transfer trolley for smooth transfer of the patient from the operating theatre to the Ingenia MRI scanner and the brachytherapy treatment room with the applicators in place.
MRI sequences for target volume delineation and applicator reconstruction
“The target definition is based on T2-weighted images. We recommend planning the sequence orientation relative to the applicator, so we perform a para-transverse imaging series, and also para-sagittal and para-coronal sequences,” says Dr. Tanderup.
“It is possible to add extra sequences to help us to better identify the position of the needles, because that dictates our ability to obtain the best accuracy for defining the source position. For complicated implants we may also acquire CT, which provides excellent visualization of needles.”
MRI parameters for the (pre) brachytherapy scans in cervical cancer patients at AUH
| Sequence | Orientation | Planning | Scan parameters Ingenia 1.5T (skin to skin) | Scan parameters Ingenia 3.0T |
| T2W TSE MultiVane XD | Para-sagittal* | Pelvic side wall (obturator muscle) | TR 4000 ms, TE 115 ms Voxels 0.85 x 0.85 x 4.00 mm | TR 3300 ms, TE 110 ms |
| T2W TSE | Para-axial* | Above uterine corpus – inferior border of symphysis pubis/entire vagina if distal vaginal involvement | TR 9772 ms, TE 90 ms Voxels 0.63 x 0.63 x 4.00 mm Scan time 4:23 min. | TR 4475 ms, TE 105 ms Voxels 0.9 x 0.9 x 3 mm Scan time 3:26 min. |
| T2W TSE | Para-coronal* | Uterine corpus – cervix – vagina – tumor | TR 4600 ms, TE 90 ms Voxels 0.9 x 0.9 x 5.00 mm Scan time 4.08 min. | TR 3575 ms, TE 110 ms Voxels 0.9 x 0.9 x 4.0 mm Scan time 2.23 min. |
*Relative to applicator
Interdisciplinary collaboration for efficient cervical cancer care
“To efficiently provide MR-guided brachytherapy we work in a multidisciplinary team,” says Dr. Tanderup. “Such a team can be set up in multiple ways, but we certainly need radiology to set up the MR sequences for high image quality, and to jointly interpret the images. Radiology expertise is also essential for our development of further advances in imaging, like the use of DCE-MRI and DWI, and the sequences for applicator reconstruction.”
“We have everything ready for international dissemination of MRI-guided brachytherapy for cervical cancer patients”
Evidence and international consensus make approach ready for dissemination
Summarizing the findings demonstrates the remarkable progress made in the past five years. Studies first found a 10% higher overall survival by adding brachytherapy to radiation therapy for cervical cancer. On top of that, more recent studies showed an additional 10% increase in overall survival for brachytherapy with MRI guidance compared to conventional brachytherapy [1,2]. The 2016 ICRU report on ‘Prescribing, recording and reporting brachytherapy for cancer of the cervix’ shows an international consensus on the approach [4].
“We have everything ready for international dissemination of MRI-guided brachytherapy for cervical cancer patients,” concludes Dr. Tanderup.
References
1. Han K, Milosevic M, Fyles A, Pintilie M, Viswanathan AN. Trends in the utilization of brachytherapy in cervical cancer in the United States. Int J Radiat Oncol Biol Phys. 2013;87:111-9.
2. Gill BS, Lin JF, Krivak TC, Sukumvanich P, Laskey RA, Ross MS, Lesnock JL, Beriwal S. National Cancer Data Base analysis of radiation therapy consolidation modality for cervical cancer: the impact of new technological advancements. Int J Radiat Oncol Biol Phys. 2014;90:1083-90.
3. Lindegaard JC, Fokdal LU, Nielsen SK, Juul-Christensen J, Tanderup K. MRI-guided adaptive radiotherapy in locally advanced cervical cancer from a Nordic perspective. Acta Oncol. 2013;52(7):1510–19.
4. International Commission on Radiation Units and Measurements. Prescribing, Recording, and Reporting Brachytherapy for Cancer of the Cervix (ICRU report 89). Bethesda: 2016.
5. Han et al. A prospective study of DWI, DCE MRI and FDG PET imaging. Radiother Oncol vol 120, 2016
6. An International Study on Magnetic Resonance Imaging (MRI)-Guided Brachytherapy in Locally Advanced Cervical Cancer (EMBRACE).
www.embracestudy.dk.
7. Sturdza A, Pötter R, Fokdal LU, Haie-Meder C, Tan LT, Mazeron R, et al. Image guided brachytherapy in locally advanced cervical cancer: Improved pelvic control and survival in RetroEMBRACE, a multicenter cohort study. RadiotherOncol 2016;120:428–33.
8. Pötter R, Dimopoulos J, Georg P, et al. Clinical impact of MRI assisted dose volume adaptation and dose escalation in brachytherapy of locally advanced cervix cancer. Radiother Oncol 83(2):148-155, 2007
9. Lindegaard JC, Fokdal LU, Nielsen SK, Juul-Christensen J, Tanderup K. MRI-guided adaptive radiotherapy in locally advanced cervical cancer from a Nordic perspective. Acta Oncol 2013;52:1510–9.
Results from case studies are not predictive of results in other cases. Results in other cases may vary.
10. Charra-Brunaud C, Harter V, Delannes M, Haie-Meder C, Quetin P, Kerr C, et al. Impact of 3D image-based PDR brachytherapy on outcome of patients treated for cervix carcinoma in France: results of the French STIC prospective study. Radiother Oncol 2012;103:305–13. doi:10.1016/j.radonc.2012.04.007
11. Rijkmans EC, Nout RA, Rutten IHHM, Ketelaars M, Neelis KJ, Laman MS, et al. Improved survival of patients with cervical cancer treated with image-guided brachytherapy compared with conventional brachytherapy. Gynecol Oncol 2014;135:231–8.
12. Haie-Meder C, Pötter R, Van Limbergen E, Briot E, De Brabandere M, Dimopoulos J, et al. Recommendations from Gynaecological (GYN) GECESTRO Working Group (I): concepts and terms in 3D image based 3D treatment planning in cervix cancer brachytherapy with emphasis on MRI assessment of GTV and CTV. Radiother Oncol 2005;74:235–45.
13. Pötter R, Haie-Meder C, Van Limbergen E, Barillot I, De Brabandere M, Dimopoulos J, et al. Recommendations from gynaecological (GYN) GEC ESTRO working group (II): concepts and terms in 3D image-based treatment planning in cervix cancer brachytherapy-3D dose volume parameters and aspects of 3D image-based anatomy, radiation physics, radiobiology. Radiother Oncol 2006;78:67–77.
14. Hellebust TP, Kirisits C, Berger D, Pérez-Calatayud J, De Brabandere M, De Leeuw A, et al. Recommendations from Gynaecological (GYN) GEC-ESTRO working group: considerations and pitfalls in commissioning and applicator reconstruction in 3D image-based treatment planning of cervix cancer brachytherapy. Radiother Oncol 2010;96:153–60.
15. Dimopoulos JCA, Petrow P, Tanderup K, Petric P, Berger D, Kirisits C, et al. Recommendations from Gynaecological (GYN) GEC-ESTRO Working Group (IV): basic principles and parameters for MR imaging within the frame of image based adaptive cervix cancer brachytherapy. Radiother Oncol 2012;103:113–22.
Results from case studies are not predictive of results in other cases. Results in other cases may vary.
Related information
with MRI (movie)
